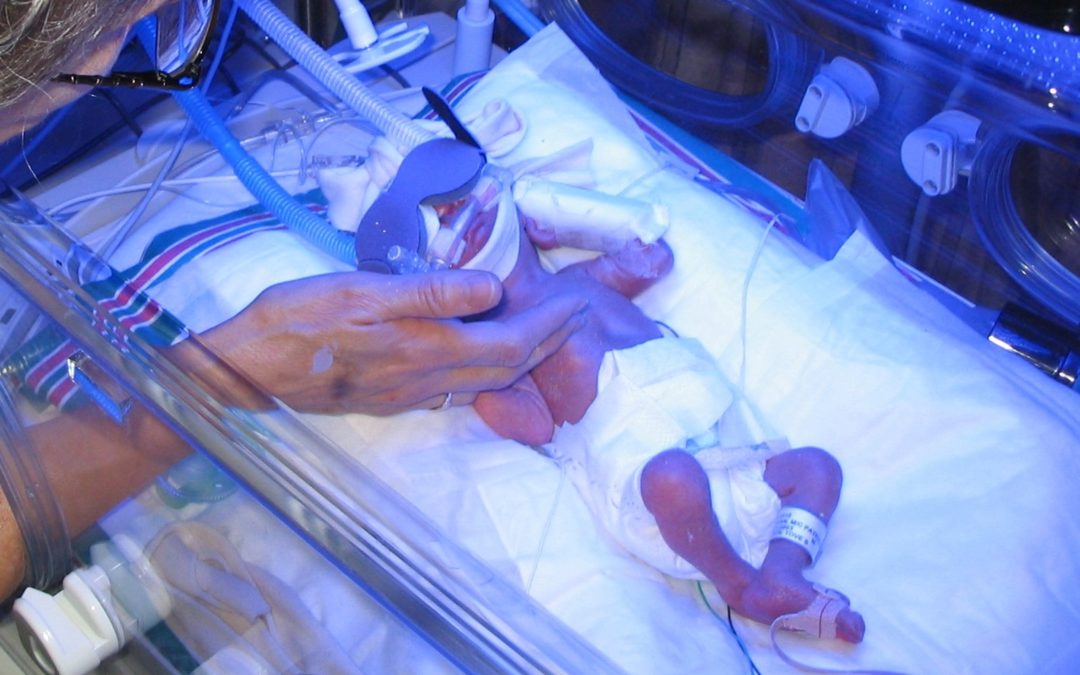
Much Wanted, Strong-Willed
When the elevator doors opened onto the floor of the neonatal intensive care unit, Mike and I were greeted by deafening sirens, flashing lights, and doctors and nurses running toward the room our son shared with several other premature babies. It was a code blue. My heart sank, and I said to my husband, “Something terrible is happening to someone’s baby!”
We walked down the hall, trying to stay out of everyone’s way, and entered the large room.
“It’s ours!” I wailed as we ran to Connor’s incubator in the corner near the window.
The top had been removed, and our tiny son was surrounded by doctors and nurses frantically trying to save his life. It wasn’t going well. He was lifeless, dark purple, his monitor showing no signs of heartbeat or breathing. He looked so alone. A doctor was trying to insert a breathing tube into his impossibly small body. I heard the doctor mutter, “I can’t get a vent!”
“Connor!” I yelled.
A nurse approached us and said, “I’m sorry, but you need to wait outside.”
She ushered us out of the room and I asked her, “What happened? He was okay when we left for lunch!”
She said he had stopped breathing—something not uncommon in the NICU. It had happened to Connor countless times in the 16 days since his birth at just 29 weeks. But in the past, the measures used to resuscitate him had worked. This time, they hadn’t. He had crashed.
Standing in the hall, Mike and I desperately prayed. After what seemed like an eternity, a doctor came out. We looked at him hopefully. He shook his head and said, “Nothing yet.”
I sank to the floor and cried, my back against the wall. Mike sat down next to me.
How many minutes had passed? About five, Mike said.
And how many had passed before we got there? No way to know, he said.
If he’s revived now, could he possibly be okay after so much time without oxygen?
My husband, a doctor who worked for that hospital and had done rotations in that NICU, assured me that some babies are fine even after a long time without oxygen. But there was fear in his eyes.
Then he jumped up. “I have to go back in and baptize him.”
It was a knife in my heart. That’s when I knew we were probably going to lose him.
When Connor was born 11 weeks early, weighing barely two pounds, all four of our parents urged us to baptize him immediately. After all, he was in intensive care on breathing equipment. It was “touch and go.”
But Mike said no. Mike had seen many NICU babies during his practice, and he said Connor looked great for a preemie. His vitals were strong, and he was gradually gaining weight from my pumped breast milk, fed to him through the tiniest tube I’d ever seen.
There was no need for a hospital baptism. Our son would have a “real” christening in a church, surrounded by loved ones, followed by a big party. Under Catholic rules, once a baby is baptized there can be no “do-over.” So we should only baptize him in the NICU if he was about to die.
And there it was. Mike believed Connor was about to die. Maybe he was already gone. Left alone in the hall while Mike ran back into the room, I sobbed and called my parents.
“Please pray! I can’t lose him now!”
I had waited so long for Connor. I met Mike when I was 37, married him when I was 38, and had Connor when I was 39. I certainly wasn’t the oldest woman ever to have a baby. But my obstetrician had warned that my “advanced maternal age” put my baby at risk for all sorts of bad things.
So I did everything right during my pregnancy—ate healthy; took prenatal vitamins; gave up caffeine, alcohol, artificial sweeteners.
But things started to go wrong early on. Just shy of three months, I was sitting in my office at Fox News Channel, preparing to anchor a live show. I stood up to head to the studio, and there was an enormous puddle of blood on my chair.
Terrified, I called my producer and said, “I think I’m having a miscarriage!”
“Stay where you are,” he replied. “I’m calling an ambulance!”
I was sure I was losing the baby. I knew heavy bleeding was a sign. When the EMTs arrived, they were sure too. They explained that there was nothing they could do to stop a miscarriage. They were taking me to the hospital just to keep me comfortable.
Miraculously, it was a false alarm. When we got to the hospital, a sonogram showed my baby, still there, with his little heart beating, fast and strong. I rejoiced with Mike and my parents, who had met me at the ER.
But I now had a glimpse of the devastation experienced by so many women. My heart aches for all of you who’ve been through that pain. I remember thinking we’ll start again. But I already loved this baby.
After that scare, I was put on home bed rest. Six weeks later, I was cleared for regular activity again. There had been no more big bleeds, and sonograms showed the baby (who we now knew was a boy!) was growing.
All seemed well.
But it wasn’t.
At 24 weeks and six days, I was vacuuming the living room of our Manhattan apartment when I felt a big gush.
I rushed to the bathroom. Mike saw me and followed.
I was relieved to tell him it was just some clear fluid pouring out of me, not blood.
He looked in the toilet and his face went pale.
“It’s amniotic fluid,” he said in a low voice. “Your water just broke.”
“What?” I scoffed, almost laughing. “I’m only at 24 weeks! What else could it be?”
“It’s amniotic fluid. We have to get you to the hospital. What do you need me to pack?”
“I don’t know!” I said. “I haven’t gotten to that part of the books yet!”
He threw some stuff in a bag, and we caught a cab to the hospital.
Once there, Mike told the reception desk that my water broke. Hearing how early I was, a doctor “explained” that it was probably just urine. It’s common for pregnant women to leak a little, due to increased pressure on their bladder.
Mike and I insisted that it was definitely not urine. But the doctor was unconvinced, and instructed me to walk laps around the floor while wearing a pad, in hopes that I would leak again so they could test the fluid.
In retrospect, this was astonishingly irresponsible advice. After several laps, I did leak again, and they analyzed the material on the pad. Discovering that it was, in fact, amniotic fluid, they put me on a bed and told me to move as little as possible.
A doctor came into our room and confirmed that my amniotic sac had ruptured, which typically leads to labor within 24 to 48 hours.
If that were to happen, she calmly rattled off a devastating list of complications our son was likely to suffer for his entire life, including breathing problems, heart abnormalities, intestinal issues, hearing and vision problems and neurological disorders.
That list is for babies born at 37 weeks or less. I was less than 25 weeks along. Babies born at this stage often didn’t even survive. And those who did struggled.
Contemplating my son’s future with severe health problems, I cried so hard my whole body was heaving and shuddering. I asked the doctor if there was anything I could do to postpone his birth. Without a trace of irony, she said it was essential that I stay positive and think happy thoughts. Oh, and try not to move or shake.
While an early rupture usually means the body is trying to push the baby out due to infection or some other complication, sometimes the sac ruptures for no apparent reason, and it doesn’t induce labor.
In those cases, the mother can sometimes stave off delivery for a week or two, despite the womb being compromised. I was not in labor—no contractions, no dilating. And there were no signs of infection or fetal distress. The doctors were already remarking that my son’s vitals were excellent given the situation. He was a fighter. So I could possibly buy him more time in the womb by staying hospitalized on strict bed rest. The average, for babies not delivered within that first one to two days, is 10 days. Some women go longer. The doctor said every day he stayed inside me would make a huge difference.
So I was wheeled to a room in the maternity ward, where I was told to stay flat on my back to eliminate downward pressure on my womb. Since my sac was ruptured, I was being given intravenous liquids to replenish the fluid, but every time it reached a certain level, it would leak out onto my pad. The sac’s fluid level was periodically measured by sonogram. It was usually between 10 and 30 percent of what it should be.
I was not allowed to sit up, other than briefly for meals. I wasn’t supposed to walk to the bathroom (a bed pan was nearby). I was given steroid shots to speed up the baby’s lung development, and antibiotics to ward off infection. Every so often, a contraption on my mattress would inflate around my legs to get the blood flowing and avoid clots. A fetal monitor was strapped across my stomach, and a separate monitor for my own heart. My temperature was taken frequently. If either of us showed signs of infection or distress, the baby would have to come out.
I was determined that this would not happen. I resolved to lay calmly on my back staring at the ceiling for as long as possible. There was flowered wallpaper trim just under the ceiling. A TV was mounted high up on the wall. I could do this. One day at a time.
I was there for 31 days.
The morning after my first night there, Mike suggested we decide on a name. So far we had only tossed around ideas, thinking we had many more months to choose one. Now it seemed we would only have days or hours.
He suggested “Connor.”
I loved it. I said, “When you go home tonight, please look up what it means.”
The next morning, Mike showed up in my room grinning.
“Connor,” he said, “means much-wanted and strong-willed.”
I smiled. “Well, I guess we have our name.”
Twenty-nine weeks and two days into my pregnancy, I lost a lot of fluid. Normally, Connor’s vitals remained satisfactory even after a gusher. Not this time. His numbers started to fluctuate. I was moved to the labor and delivery ward for the night, just in case.
In the middle of that night, I awoke concerned. I glanced at the monitor. Connor’s heart rate was not showing up. Not a big deal. Very often while I slept, the fetal monitor would shift off the baby, and I’d lose the heartbeat. After 31 days in the hospital, I knew how to slide the monitor around on my stomach until I found the beat again.
But this time no matter where I rolled that monitor, I could not find a heartbeat. I called to Mike, who was sleeping on the chair. He slid the monitor all around, then hurried out of the room.
Moments later, a team of doctors rushed in with a sonogram machine, Mike in tow. Within seconds, they had the device on my stomach, and I could see Connor’s tiny form on the screen. What I could not see was a heartbeat. There was a faint blip, every so often. Way too weak and sluggish.
The doctors urgently wheeled me out of the room on my bed, saying, “Your baby is going to be delivered right now by C-section.”
As we hurtled down the hall, an anesthesiologist fired off questions about allergies and reactions. Then I was in the brightly-lit operating room, feeling like I had failed my son. I was still 11 weeks early. Connor had been “measured” by sonogram earlier that day. It’s not exact, but they estimated his weight at less than two pounds. The doctors had told us outcomes were much better for babies born over two pounds. He was too small. It was too soon.
Mike appeared at my side in scrubs. I told him, “I love you.”
He said, “I love you too.”
I was awake through it all, and after mere minutes, a voice from the other side of the curtain said, “He’s out! Good tone!”
He was alive! I heard no crying, but I knew from the preemie book I’d read that most premature infants are too weak to cry.
Mike peeked around the curtain and looked pleased.
“He looks great! Big!”
I yelled, “Hi Connor! I’m your mommy! I love you!”
Then they whisked him out of the room.
Connor weighed two pounds, six ounces at birth. That’s very small, but since we were expecting a baby under two pounds, we were thrilled. His Apgar scores were good, and his vital stats were decent, considering the circumstances.
But he was on breathing equipment known as CPAP (continuous positive airway pressure). And it seemed like every inch of his tiny body had something taped to it and wires coming out of it. His monitor beeped frequently, alerting the hospital to bradycardias (heart slowdowns requiring intervention), apnea (slowed breathing), and “de-sats” (decreased oxygen saturation).
He was jaundiced, so he had to lie blindfolded under special lights for six days, which is not uncommon, but it just increased his discomfort. A brutal spinal tap when he ran a fever added insult to injury.
I spent most of every day at Connor’s side. Mike and I were allowed to hold him for brief periods at first, then longer periods as he got stronger. I sang to him and read him stories. Relatives would visit, speaking at first into the holes of his incubator, letting him grab their fingers, later holding him when allowed.
The nurses taught me how to “stimulate” him to get his heart back up to speed when his alarm went off. Sometimes loudly yelling his name was enough. Other times he needed his foot squeezed or his back tapped. As the days went by, his monitor was beeping less, and he required less stimulation to be revived.
Things were moving in the right direction.
Until they weren’t.
After about two weeks, things started going backwards. He started de-saturating more frequently, and it was taking longer to revive him. The doctors were not concerned. They said there’s often a “honeymoon phase” after which a preemie might have a few setbacks, but it’s nothing to worry about.
But it got alarmingly worse. The de-sats were downright scary. He wasn’t responding to simple stimulation. The nurses had to resort to more dramatic interventions. One time his color went from gray to blue, and he required “bagging” (an inflating bag to push oxygen into a mask placed over his face).
Connor’s whole body looked tense, and his facial expression, which had been pretty relaxed, was now a constant wince. The doctors suspected infection and put him on antibiotics, but he continued to go downhill.
Finally on day 16, a nurse persuaded the doctors Connor needed a blood transfusion. It was begun a few hours later. The doctor said it would take a few hours for the transfusion to improve Connor’s condition, but we were relieved knowing the “cure” was at last underway.
Having barely left Connor’s side for days as his condition deteriorated, I now felt comfortable getting a quick lunch with Mike across the street. So we left Connor in his incubator.
We returned from lunch to find our infant son coding. After we were escorted from the room, precious minutes passed as we waited in the hall, aware that each passing second meant a potentially worse future for Connor, if he survived at all.
As the doctors struggled to save Connor, Mike re-entered the room and grabbed one of our bottles of holy water from the nightstand next to his incubator.
“Excuse me,” he said, trying to clear a path between two nurses to stand beside Connor’s unresponsive body.
“He’s baptizing him!” one said. “Let him through.”
Mike quickly prayed, “I baptize you in the name of the Father, Son, and Holy Spirit.”
Then he left. Waiting in the hall, I scanned Mike’s face for a sign of hope.
“Still nothing,” he said.
“It’s been too long,” I exclaimed. “Too long!”
But soon a doctor emerged. Removing his mask, he said, “He’s back.”
“Thank God!” we both exclaimed.
The doctor continued, “He’s intubated, but so far he looks good. Sometimes when babies emerge from an episode like this, there are indications the oxygen loss may have caused brain damage. But once we got an airway into your son, his color went back to pink, and he started tugging at the breathing tube, which is a great sign. We literally had to fight with him to stop him from yanking out the vent. He’s a tough cookie. I’m cautiously optimistic.”
We hurried to Connor’s Isolette, and there he was—pink again, breathing again, looking at us through the glass when we called his name. He looked exhausted, and the ventilator looked horribly uncomfortable, but it seemed miraculous that this was the same baby who 10 minutes earlier was ash-colored and showed no signs of life.
I told him I loved him, my arms draped over the top of the incubator, my face pressed against the glass, tears streaming down my cheeks.
Much wanted. Strong willed. Connor.
The preceding is an abridged excerpt from Patti Ann Browne’s upcoming memoir: Write Your Own Story: How I Took Control by Letting Go. (Post Hill Press, April 26, 2022). Available on Amazon, Barnes & Noble and Books a Million.
“Beautiful, honest and emotional.” – JANICE DEAN, Fox News Senior Meteorologist and NY Times bestselling author
“Incredibly moving…a real page turner…so powerful.” – GREG KELLY, Newsmax TV host, radio & podcast host, retired U.S. Marine
“A must read!” – PETER KING, former US Congressman
“Funny, self-deprecating and heart wrenching.” – DAVID G. BONAGURA, Jr., author of “Steadfast in Faith” and “Staying with the Catholic Church”
“Patti Ann takes you on a journey of her personal and professional triumphs and disappointments.” – CARL DENARO, author of “The Son of Sam and Me”